Health April 7, 2026
Biosimilars vs Generics: Key Differences Explained
You might have noticed your pharmacist asking if you want the "generic version" of a pill, and you probably just said yes. It's a routine part of healthcare. But when it comes to complex injections or biologics, the conversation changes. Suddenly, you're hearing about biosimilars is a highly similar but not identical version of a reference biologic drug. It sounds like a generic, but in the world of medicine, the difference between a "generic" and a "biosimilar" is as huge as the difference between a bicycle and a jet engine.
The Core Difference: Simple Chemistry vs. Living Cells
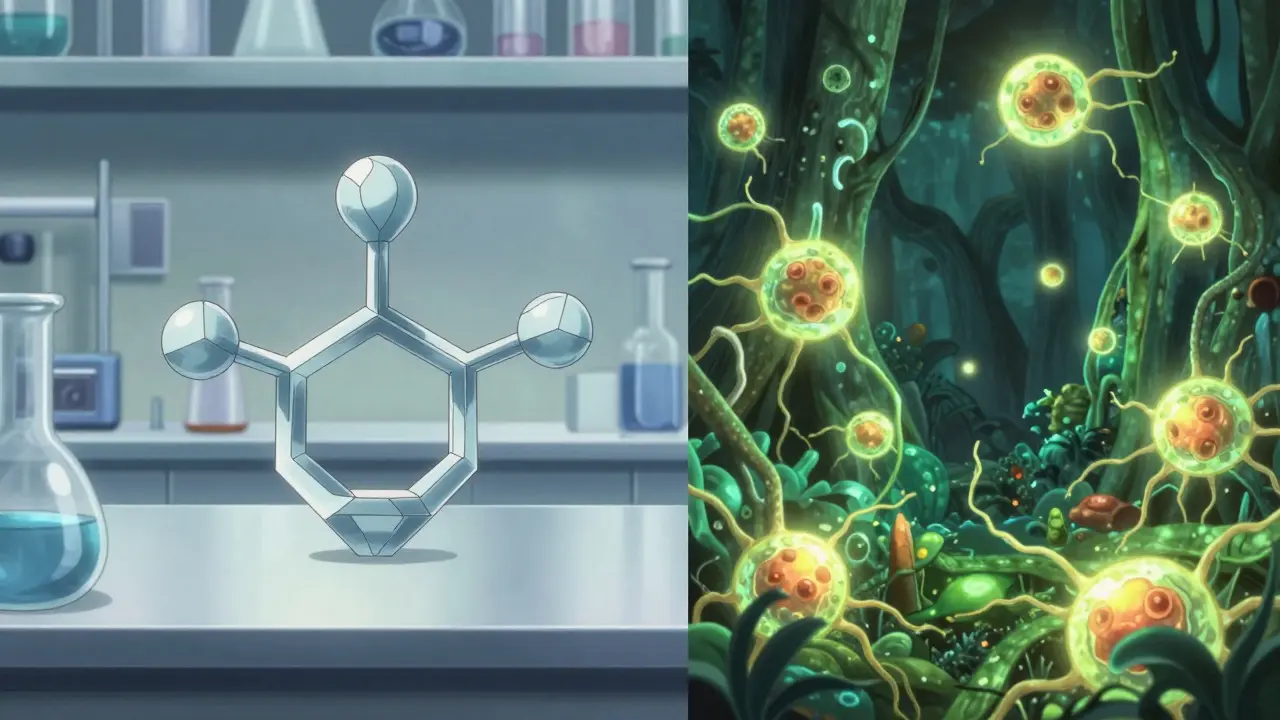
To understand why we have two different terms, we have to look at how these drugs are made. A Generic Drug is a small-molecule medication. Think of it like a simple recipe for a cake; if you have the exact same ingredients and follow the steps, you get the exact same cake every time. These drugs are synthesized from chemicals in a lab. For example, aspirin has a molecular weight of just 180 daltons. Because the structure is so simple, a generic manufacturer can make a version that is chemically identical to the brand name.
Biosimilars, however, are large-molecule proteins. They aren't made by mixing chemicals; they are grown using living organisms, like plant or animal cells. Imagine trying to replicate a living forest instead of a cake. Even if you use the same seed and soil, no two forests are exactly identical. These proteins are massive-often 1,000 to 5,000 times larger than small-molecule drugs. A monoclonal antibody like infliximab has a molecular weight of around 148 kilodaltons. Because they come from living cells, there are always tiny, natural variations between batches.
How Approval Works: Identical vs. Highly Similar
Because the science is different, the FDA (U.S. Food and Drug Administration) uses two different rulebooks for approval. For generics, the goal is bioequivalence. This means the generic drug must be absorbed into the bloodstream at the same rate and to the same extent as the original. Once that's proven, the drug is considered interchangeable.
Biosimilars can't be "identical" because of their biological nature. Instead, the FDA requires them to be "highly similar." This means the manufacturer has to prove there are no clinically meaningful differences in safety, purity, and potency. To do this, they often have to test 200 to 300 different quality attributes. While generics can be approved with simple pharmacokinetic studies, biosimilars often require animal studies and limited clinical trials to ensure they don't trigger an unexpected immune response (immunogenicity).
| Feature | Generic Drugs | Biosimilars |
|---|---|---|
| Molecular Structure | Small molecule (simple) | Large protein (complex) |
| Production Method | Chemical synthesis | Living cell cultures |
| Relationship to Original | Chemically identical | Highly similar |
| Substitution | Automatic at pharmacy | Requires "Interchangeable" status |
| Typical Cost Savings | 40% to 50% lower | 15% to 33% lower |

The Substitution Puzzle: Can You Just Swap Them?
This is where patients often get confused. In most U.S. states, a pharmacist can automatically swap a brand-name drug for a generic without calling your doctor. This is called automatic substitution. It's safe because the drugs are identical.
Biosimilars don't work that way. Most biosimilars require the doctor's explicit approval to switch. There is a special category called Interchangeable Biosimilars. These have gone through extra testing to prove that switching back and forth between the original and the biosimilar doesn't affect the patient's health. Even so, this is rare. As of late 2023, only 7 out of 42 approved biosimilars in the U.S. had this status. If your drug isn't labeled as interchangeable, your doctor has to make the call to switch you.
Why Biosimilars Cost More to Make (and Buy)
If you look at the price tag, generics are almost always cheaper than biosimilars. This isn't because the companies are greedy; it's because of the sheer cost of development. Bringing a generic to market might cost between $2 million and $5 million. Bringing a biosimilar to market? That can cost between $100 million and $200 million.
One big reason for this is the "secret sauce" problem. When a company makes a generic, they just copy the chemical formula. But the process for growing a biologic drug in a living cell is proprietary. Biosimilar companies can't just see the original manufacturer's manual; they have to reverse-engineer the process to get a product that is "highly similar." This extra work means the price drops for consumers are smaller-usually 15% to 33% compared to the 50% drop seen with generics.

Real-World Impact: Oncology and Immunology
You'll see biosimilars most often in high-cost areas like cancer treatment (oncology) and autoimmune diseases (immunology). For example, drugs that treat rheumatoid arthritis, like adalimumab (brand name Humira), have seen biosimilar versions enter the market. These alternatives are critical because the original biologics can cost tens of thousands of dollars per year.
However, switching isn't always a slam dunk. The American College of Rheumatology suggests that while starting a new patient on a biosimilar is fine, switching a patient who is already stable on a reference product should be done with caution and close monitoring. There is always a small risk that the body will react differently to a slightly different protein structure.
The Road Ahead: Patent Thickets and Future Access
The growth of biosimilars has been slowed by something called "patent thickets." This happens when a brand-name company files hundreds of small patents to block competitors. AbbVie did this with Humira, filing over 240 patents to keep competitors at bay for years. Despite this, the tide is turning. The Inflation Reduction Act of 2022 is expected to lower out-of-pocket costs and push more people toward these affordable alternatives.
We are also seeing the rise of "bio-super-similars"-products that aren't just similar but might actually offer improved properties over the original. As more patents expire for major drugs like Stelara and Eylea, the market will shift from a few expensive options to a competitive landscape where patients have more choices and lower bills.
Is a biosimilar exactly the same as a generic?
No. A generic drug is a chemically identical copy of a small-molecule drug. A biosimilar is a highly similar version of a large-molecule biologic drug. Because biosimilars are made from living cells, they can never be 100% identical, but they are designed to have no clinically meaningful differences in safety or effectiveness.
Can my pharmacist switch my biologic to a biosimilar automatically?
Usually, no. Only biosimilars that have been specifically designated as "interchangeable" by the FDA can be substituted without the doctor's intervention. Most biosimilars require a new prescription or a doctor's approval to switch.
Are biosimilars safe to use?
Yes. To be approved, biosimilars must undergo rigorous testing to prove they are as safe and effective as the original reference product. The FDA ensures there are no clinically meaningful differences in how the drug works or its safety profile.
Why are biosimilars not as cheap as generics?
Developing a biosimilar is far more expensive than a generic. While a generic might cost a few million dollars to develop, a biosimilar can cost up to $200 million due to the complexity of working with living cells and the extensive clinical testing required.
Where can I find a list of approved biosimilars?
The FDA maintains the "Purple Book," which is the official catalog of licensed biological products, including biosimilars and interchangeable products. This is different from the "Orange Book," which lists generic drugs.
Write a comment
Items marked with * are required.




12 Comments
Rauf Ronald April 9, 2026 AT 07:15
The distinction between small-molecule synthesis and protein expression is a huge point here. A lot of people don't realize that biologics are basically grown, not mixed, which is why the purity standards are so insane. It's awesome to see more biosimilars hitting the market because it genuinely breaks the monopoly that some of these big pharma companies have had for decades. If you're looking into this, check out the Purple Book for the most current data on interchangeability since that's where the real pharmacy-level changes happen. Let's keep pushing for more access to these life-saving meds!
Grace Lottering April 10, 2026 AT 00:54
Big Pharma just wants us dependent on their 'secret sauce' to keep the prices high.
Del Bourne April 10, 2026 AT 13:43
It is quite fascinating how the FDA handles the 'highly similar' designation. Since the molecular structures are so massive, achieving a perfect 1:1 chemical copy is physically impossible. Therefore, the focus shifts to clinical outcomes-ensuring that the biological activity and the safety profile remain consistent. For those managing chronic conditions, it is always best to discuss the specific brand of biosimilar with your specialist to ensure a smooth transition.
GOPESH KUMAR April 12, 2026 AT 05:38
Typical oversimplification. You act like the 'patent thickets' are some grand mystery when it's just basic corporate greed and legal maneuvering. The irony is that these 'bio-super-similars' will probably just create another cycle of overpriced patents in ten years. It's a loop of artificial scarcity. People think they're getting a deal with a 15% discount, but in reality, they're just paying a slightly lower premium for a system that's fundamentally broken. We're just swapping one corporate master for another while pretending the science is the only hurdle.
Nathan Kreider April 13, 2026 AT 11:49
I really hope this means prices go down soon for everyone. It's so hard for some families to afford these drugs.
Darius Prorok April 13, 2026 AT 20:06
Everyone knows the Purple Book is where you look for this stuff. Just check the book and you're done.
Vivek Hattangadi April 15, 2026 AT 04:00
I totally agree with the point about the Inflation Reduction Act! It's such a game changer for accessibility. We should all be looking at how these policies can be expanded to other high-cost treatments too. Imagine if we could apply this level of competitive pressure to every specialty drug on the market. It would be a massive win for patients everywhere, and I'm really excited to see how the market evolves over the next couple of years. Let's keep supporting these moves toward lower costs!
Victoria Gregory April 16, 2026 AT 02:55
Wow!!! The forest analogy is just so beautiful and makes it so easy to understand 🌲✨ I love how science can be explained like this!!! It really makes me feel more peaceful about the idea of using a biosimilar if the 'forest' is basically the same 🌸💖
Laurie Iten April 16, 2026 AT 15:32
the idea of a bio-super-similar is an interesting philosophical shift from copying to improving
maybe the goal shouldnt be similarity but evolution
Kathleen Painter April 16, 2026 AT 19:10
I've spent a lot of time talking with people in my community who have had to switch medications, and the anxiety surrounding that transition is very real. It's important to remember that while the science says these drugs are highly similar, the psychological impact of switching a medication that has kept you stable for years can't be ignored. I think we need to focus more on the patient support side of things-making sure there's a bit more hand-holding from the medical staff during that first month of a switch. It's not just about the molecule, it's about the person taking it, and creating a space where patients feel heard and safe during the process is just as important as the drug's efficacy. We should really strive for a healthcare model that prioritizes that emotional transition alongside the clinical one, ensuring nobody feels like a guinea pig in a corporate cost-cutting experiment, even if the drug is technically safe.
Rupert McKelvie April 17, 2026 AT 09:29
It is heartening to see the progress being made in reducing the cost of these essential treatments. The transition to biosimilars represents a significant step forward for public health globally.
charles mcbride April 18, 2026 AT 15:15
The shift toward these alternatives is certainly a positive development for the healthcare system. It is encouraging that we are moving toward a more sustainable pricing model for biologics.