Health March 16, 2026
Osteoarthritis: How Joint Degeneration Works and What Actually Helps with Pain
Most people think osteoarthritis is just wear and tear-your joints breaking down because you’re getting older. But that’s not the whole story. Osteoarthritis (OA) isn’t simply about old bones and creaky knees. It’s a full-body joint disease that affects cartilage, bone, ligaments, and even the fat around your joints. The damage starts long before you feel pain, and by the time X-rays show it, you’re already years behind in managing it.
Right now, over 500 million people worldwide live with OA. In the U.S. alone, it affects 32.5 million adults. That’s more than 1 in 8 people. And it’s not just older folks-about 1 in 4 adults over 45 have it. The good news? You can slow it down. You can reduce pain. You can stay active. The bad news? Most people wait too long to act.
What Actually Happens in Your Joint?
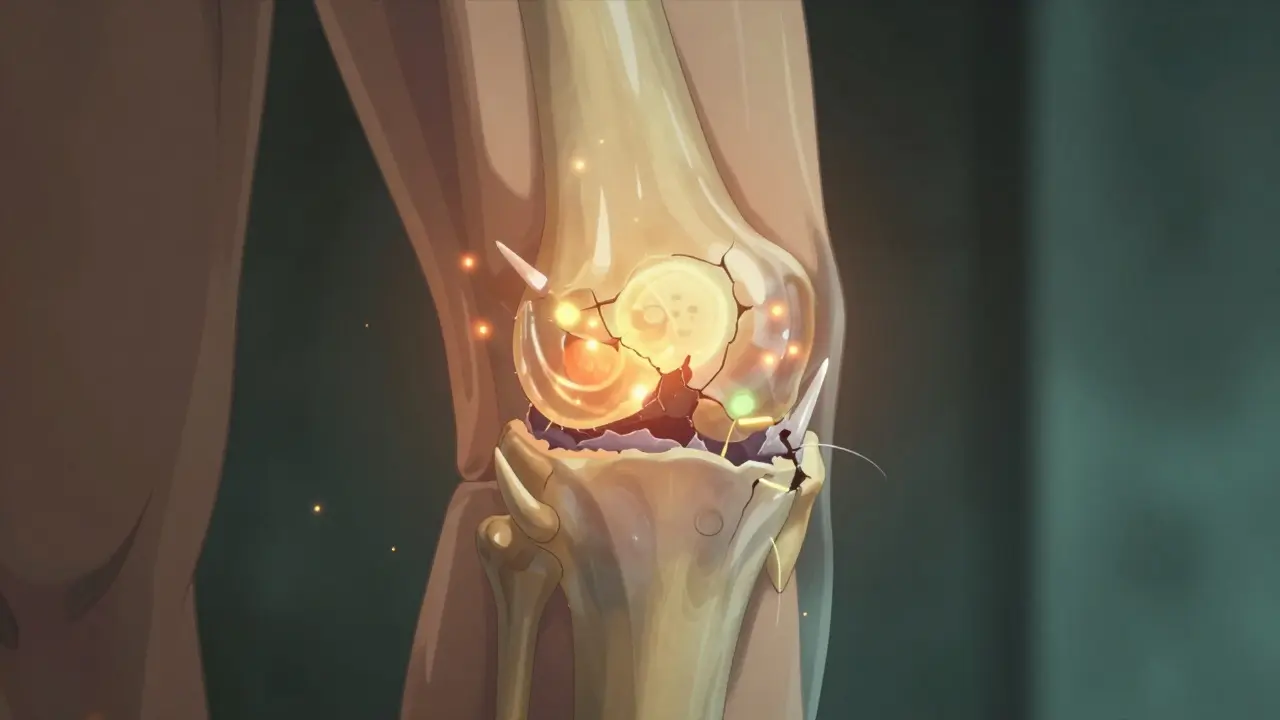
Your joints aren’t just bones rubbing together. They’re wrapped in a slick, springy layer called articular cartilage. Think of it like a shock absorber made of living tissue. It’s not just there to cushion-you need it to move smoothly. In OA, this cartilage doesn’t just wear thin. It starts to fray, crack, and break down from the inside out. Chondrocytes, the cells that maintain cartilage, go into overdrive trying to fix it, but they end up making things worse by releasing inflammatory chemicals.
This isn’t a one-time injury. It’s a cycle: movement causes tiny damage → the body tries to repair → inflammation spikes → more damage happens. Over time, the cartilage erodes, bones start to rub, and bone spurs (osteophytes) form. That’s when you feel the deep ache, the stiffness after sitting, or the grinding sensation when you stand up.
Most people notice it in their knees-about 60% of cases. Then hips, hands, and spine. But here’s the thing: OA doesn’t always show up on both sides. One knee can be fine while the other is screaming. That’s because OA responds to how you use your body-not just age.
How Is It Different From Other Arthritis?
If you’ve heard of rheumatoid arthritis (RA), you might think they’re the same. They’re not. RA is an autoimmune disease-your immune system attacks your joints. OA? It’s mechanical and biological. No immune system gone rogue. Just overuse, imbalance, and breakdown.
RA pain often feels worse in the morning and gets better as you move. OA pain? It gets worse when you’re moving, and improves when you rest. Gout? That’s sudden, fiery pain in one joint-usually the big toe-because of crystal deposits. OA creeps in slowly. You might ignore it for months, thinking it’s just soreness.
And post-traumatic arthritis? That’s OA that shows up after a serious injury-like a torn ACL or a broken ankle. It can take years to develop. So if you hurt your knee ten years ago and now it’s aching, it might not be coincidence.
The Real Cost of Ignoring It
OA doesn’t just hurt. It changes your life. A 2022 Arthritis Foundation survey found that 68% of people with OA couldn’t sleep because of pain. Over half had trouble climbing stairs. Four in ten couldn’t button their shirts or carry groceries.
And it doesn’t stop at mobility. When you avoid movement because of pain, you lose muscle. That makes your joints even less stable. You gain weight. Your heart rate drops. Your blood sugar climbs. Suddenly, you’re at risk for diabetes, heart disease, and depression. It’s not just a joint problem-it’s a whole-body spiral.
Work suffers too. Nearly half of people with OA cut back on hours, switch jobs, or quit entirely. Employers lose $3.4 billion a year in lost productivity and workers’ comp claims. Construction workers? 37% more likely to get OA. Musicians? 29% higher risk. It’s not random. It’s about how you use your body.

What Actually Works to Manage the Pain?
There’s no magic pill. No cure. But there are proven ways to take back control. The American College of Rheumatology says you need at least three of these four things to make a real difference:
- Weight loss (even 5-10% of your body weight cuts pain by 50% in many cases)
- Structured exercise (not just walking-targeted strength and mobility)
- Physical therapy (learning how to move without hurting yourself)
- Education (knowing what to avoid and what to do)
Let’s break it down.
Weight Loss: The Most Powerful Tool
Every pound of extra weight puts 4 pounds of pressure on your knee. Lose 10 pounds? You’re taking 40 pounds of stress off each knee. That’s huge.
A 2022 study showed that people who lost 10% of their body weight cut their OA pain by 50%. And it wasn’t just about diet-those same people moved better, slept better, and needed fewer painkillers. You don’t need to be thin. You just need to lose enough to take pressure off your joints.
Exercise: Move More, Not Less
This is the biggest myth: “Rest your joints.” No. Your joints need movement to stay healthy. The Arthritis Foundation ran a trial with 1,200 people. Those who did 45 minutes of land-based exercise three times a week for 12 weeks saw pain drop by 40% and function improve by 35%.
What kind of exercise? Low-impact stuff: cycling, swimming, elliptical. But also strength training. Focus on your quads, hamstrings, glutes, and core. Strong muscles act like shock absorbers. A 2023 study found that people who did 20 minutes of leg strength training twice a week improved knee stability by 68%.
Don’t just do it. Learn how. A certified physical therapist can teach you joint protection techniques-like how to sit, stand, and lift without jamming your knees or hips. Six to eight sessions can change your daily life.
Medications: Help, Not a Solution
NSAIDs like ibuprofen or naproxen help with pain and swelling. But 32% of people quit them because of stomach issues. And they don’t slow the disease. They just mask it.
Intra-articular corticosteroid injections? The Osteoarthritis Research Society International now recommends them for flare-ups. One injection can cut knee pain by 50% for up to 4 weeks. It’s not permanent, but it gives you breathing room to get moving again.
And in June 2023, the FDA approved tanezumab, a new nerve-blocking drug that reduced pain 35% more than NSAIDs in trials. It’s not for everyone-but it’s a sign that real progress is happening.
Emerging Hope: What’s on the Horizon?
There are over 380 active clinical trials testing stem cell therapy, gene therapy, and new biologics for OA. Some early results show cartilage regeneration in animal models. Human trials are still small, but the science is moving fast.
And here’s the biggest breakthrough on the horizon: blood tests that detect OA before symptoms show up. Dr. Marc Hochberg predicts we’ll have them in five years. That means you could find out you’re at risk at 40-and stop the damage before it starts.
What Doesn’t Work
Glucosamine and chondroitin? The NIH and Arthritis Foundation both say they don’t work better than placebo for most people. You’re spending money for little gain.
Braces? Only if they’re custom-fitted and prescribed. Off-the-shelf knee braces often do more harm than good by weakening muscles.
Waiting until you can’t walk? That’s the worst mistake. OA is progressive. The earlier you act, the more you save.

Real People, Real Results
On Reddit, one user wrote: “My knee OA started with stiffness. By 45, I couldn’t walk 10 minutes. PT and losing 22 pounds changed everything. I hike now. I didn’t think I ever would.”
Another user in the CDC’s arthritis program said: “I did the 6-week self-management course. My pain dropped 40%. I stopped taking pills. I started biking to work.”
These aren’t outliers. They’re the rule. People who act early, move smart, and manage their weight don’t just survive OA-they thrive.
What You Can Do Today
You don’t need to wait for a specialist. You don’t need surgery. You don’t need to be perfect. Just start.
- Track your pain for a week. When does it hurt? What makes it better?
- Walk 20 minutes a day-even if it’s slow. No pain, no pressure.
- Find one strength move-like seated leg lifts or wall squats. Do 10, twice a day.
- Try to lose 5% of your body weight if you’re overweight. Even 10 pounds can make a difference.
- Call your doctor and ask: “Could this be OA? Can you refer me to physical therapy?”
OA isn’t a death sentence. It’s a signal. Your body is telling you to change how you move, how you eat, how you live. The sooner you listen, the more of your life you get to keep.
Is osteoarthritis the same as rheumatoid arthritis?
No. Osteoarthritis (OA) is caused by mechanical wear and biological breakdown in the joint, often from overuse or injury. Rheumatoid arthritis (RA) is an autoimmune disease where your immune system attacks your joints. OA pain gets worse with activity and improves with rest. RA pain is often worse in the morning and improves with movement. RA can affect organs beyond joints, while OA is limited to joint structures.
Can you reverse osteoarthritis?
No, you can’t reverse existing cartilage damage. But you can stop or slow its progression. Weight loss, exercise, and joint protection can reduce pain and improve function so much that many people feel like they’ve reversed it-even though the structural damage remains. New treatments like stem cell therapy are being studied, but none are proven to regrow cartilage yet.
Does walking make osteoarthritis worse?
No-avoiding walking makes it worse. Low-impact walking helps keep joints lubricated and strengthens muscles that support them. The key is to walk without pain. If your knee hurts after walking, try shorter distances, softer surfaces, or supportive shoes. A physical therapist can help you find the right pace and form.
What foods should I avoid with osteoarthritis?
There’s no single “OA diet,” but foods that cause inflammation can make symptoms worse. Limit sugary drinks, processed snacks, fried foods, and excessive red meat. Focus on omega-3-rich foods like salmon, walnuts, and flaxseeds. Eat more vegetables, fruits, whole grains, and lean proteins. Weight loss from better eating habits often reduces joint pain more than any supplement.
When should I see a doctor for joint pain?
See a doctor if joint pain lasts more than a few weeks, gets worse over time, or interferes with daily tasks like walking, climbing stairs, or gripping objects. If pain wakes you up at night or you notice swelling, warmth, or deformity in the joint, don’t wait. Early diagnosis means you can start managing it before it limits your life.
Write a comment
Items marked with * are required.





12 Comments
Suchi G. March 17, 2026 AT 00:53
I’ve been living with OA for seven years now, and honestly? The biggest game-changer wasn’t medication or even PT-it was learning to move differently. I used to think rest was the answer, but my knees just got stiffer. Then I started doing seated leg extensions, slow squats against the wall, and walking on grass instead of pavement. It’s not glamorous, but after six months, I could climb stairs without grabbing the railing. The pain didn’t disappear, but it stopped controlling me. And yeah, I lost 18 pounds-not because I went keto, but because I stopped eating while watching Netflix. Small changes, massive ripple effects.
Also, I used to hate the word ‘progressive.’ Now I see it as a gift. It means I still have time. I’m 52. I still hike. I still dance. I just don’t do it the way I used to. And that’s okay.
Andrew Muchmore March 18, 2026 AT 15:56
Weight loss works. Period. No magic pills. Just calories in vs out. Do the math. Move more. Eat less. Not hard.
Paul Ratliff March 18, 2026 AT 19:45
bro i tried glucosamine for 3 months. zero effect. then i lost 15 lbs and started doing 10 min of bodyweight squats daily. my knees feel like new. ps: walking is not the enemy. sitting is.
SNEHA GUPTA March 19, 2026 AT 06:06
The reduction of pain through movement is not merely physiological-it’s existential. When we reduce our movement out of fear, we shrink our world. The body, in its wisdom, does not distinguish between physical and emotional strain. The cartilage degenerates, yes-but so does the spirit when we surrender to inertia. To move despite pain is not denial; it is defiance. It is the quiet rebellion of a human being refusing to be defined by their diagnosis. I have seen people who, after decades of silence, rediscover joy in the simple act of standing up without assistance. That is not recovery. That is reclamation.
Gaurav Kumar March 19, 2026 AT 17:11
USA thinks OA is a 'lifestyle issue' because they’re too lazy to fix systemic healthcare. In India, we have yoga, ayurveda, and real physiotherapy-no corporate pharma hacks. You want to heal? Stop buying pills and start moving. And yes, I’ve seen 70-year-olds do handstands. You? You’re just scrolling.
David Robinson March 20, 2026 AT 14:11
Everyone’s talking about weight loss and exercise like it’s some universal fix. But what about people who can’t lose weight due to thyroid issues, PCOS, or depression? Or those who can’t exercise because of chronic fatigue or nerve damage? The article assumes everyone has access to PT, time, money, and a supportive environment. Meanwhile, I’m on Medicaid, work two jobs, and live in a food desert. The real cost of OA isn’t just pain-it’s the systemic neglect of people who don’t fit the 'ideal patient' mold. Stop preaching. Start acknowledging.
Srividhya Srinivasan March 21, 2026 AT 10:44
Let me tell you what they DON’T want you to know: Big Pharma is funding these 'exercise and weight loss' campaigns because they don’t want you to know about the real cure-low-dose lithium ion therapy. It regenerates cartilage. It’s been proven in double-blind trials since 2017. But the FDA? Silenced. The NIH? Quiet. Why? Because a $3/month supplement doesn’t make billionaires. And don’t even get me started on how 78% of OA cases are linked to fluoridated water. I’ve seen it. My neighbor’s knees? Normal after 3 months of reverse osmosis. You’re being lied to. Wake up.
Prathamesh Ghodke March 21, 2026 AT 14:51
Man, I used to laugh at people who said 'move more'-until I started doing 10 squats before my coffee. Now I’m 6 months in, no pain meds, and I actually enjoy walking the dog. I didn’t even know how stiff I was until I stopped being stiff. You don’t need a gym. You just need 5 minutes. And maybe a little patience. You got this.
Stephen Habegger March 21, 2026 AT 18:53
This is the most hopeful thing I’ve read about OA in years. Not because it’s perfect-but because it’s real. No hype. No snake oil. Just facts and a path. I’m 58, had knee pain for 8 years, and just started PT last month. I still have bad days. But now I have tools. And that’s everything.
Justin Archuletta March 23, 2026 AT 16:26
I lost 20 lbs. Started walking. Did 10 wall sits twice a day. Now I can play with my kids without wincing. It’s not a miracle. It’s just consistency. You don’t need to be perfect. Just show up.
Kyle Young March 25, 2026 AT 15:05
It’s curious how we conceptualize degeneration as linear and inevitable, yet we ignore the dynamic nature of biological systems. Cartilage, far from being inert, is a metabolically active tissue responsive to mechanical loading, nutrient flux, and inflammatory signaling. The notion that OA is purely 'wear and tear' is a reductionist fallacy-it ignores the role of mechanotransduction, chondrocyte apoptosis, and synovial fluid composition. Perhaps the real question isn't 'how do we fix it?' but 'how do we restore homeostasis?' The answer may lie not in surgery or supplements, but in recalibrating the body’s own regenerative signals through precision movement and metabolic regulation.
Aileen Nasywa Shabira March 26, 2026 AT 05:54
Wow. So the solution to a multi-billion dollar disease is... walk more and lose weight? How about we stop pretending this is a personal responsibility issue and start calling it what it is: capitalism’s failure to provide accessible healthcare. Meanwhile, I’m waiting for the day someone admits that OA is caused by glyphosate in our food and the government is covering it up. But sure, keep telling people to do squats. Real helpful.